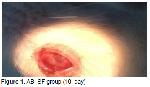
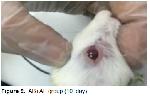
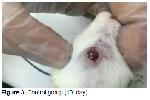
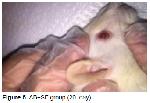
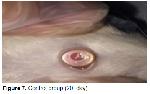
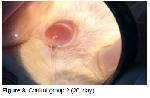
Inflammation of the cornea, which is characterized by tissue loss both in the corneal epithelium and stroma is called ulcus cornea (corneal ulcer) and it does not heal spontaneously. Causes of a corneal ulcer (ulcus cornea) are divided into two groups, as exogenous and endogenous. Often, eye trauma is considered to be a major cause of ulcus cornea formation in domestic animals. Sometimes, endogenous causes are also observed
1,2.
Bacteria rarely cause corneal ulcers although they have a primary role in corneal infections. Entropion, ectropion, distichiasis, keratoconjunctivitis sicca, foreign body sting in the cornea, conjunctival lithiasis, eyelid tumors, chemical burns, ectopic ciliate, canine juvenile disease, mycotic factors, and immune system disorders can also cause ulcus cornea 3,4.
The corneal epithelium is highly resistant to infections when the eye is not traumatized and the integrity of the cornea is not compromised. When there is an injury due to direct or indirect factors disrupting the integrity of the epithelium, the passage of microorganisms through the corneal epithelium is facilitated and this may lead to corneal ulceration. If corneal defects are not treated early or if there is no appropriate treatment; ulcus cornea may develop in a very short period of time, reaching the deep layers of the cornea and leading to major complications such as corneal vascularization, uveitis, panophthalmia or even corneal perforation 2,5,6.
Treatment can be medical or surgical. In order to reduce the pain and treat the infection; locally applied medications, anticollagenase drugs (acetylcysteine, cysteine, sodium EDTA, calcium EDTA, progesterone, medroxyprogesterone, sodium ascorbate, sodium citrate, penicillamine, tetracycline, thiol peptides, aprotinin and polysulfate glycosaminoglycan, heparin, and autogenous blood serum), and vitamins (A, B2, B12, C) are administered to patients as effective modes of medical treatment 2,4,7-9.
Amniotic membrane and amniotic fluid accelerate epithelization, prevent protein and fluid loss at the wound surface, increase fibroblastic activity, and reduce adhesion formation; as well as having antibacterial, antioxidant, and non-immunological effects 10-13.
The amniotic membrane was first used by Davis in 1910 for skin transplantation. The use of amniotic membranes in ophthalmology was first introduced by De Rotthile. The researcher used a newly acquired chorion layer in 1940 for the treatment of conjunctival epithelial defects, but no significant success was achieved. Later studies have shown that amniotic fluid and amnion membranes have been successfully used in conjunctiva pterygium surgery, filtering surgery, and symblepharon therapy, and for the treatment of chemical burns, periocular surface neoplasms, bleb leaks, conjunctival chalazion, entropion, and cicatrizing conjunctivitis 12,13.
Free oxygen radicals (FOR) have been reported to play a major role in the development of tissue damage and disease in many organs, including the eye. Despite the diversity, widespread distribution, and highly effective activities of antioxidant molecules against the free radicals in cells and tissues; this defense system may sometimes become insufficient; resulting in macromolecular damage. The commonly known FOR include hydrogen peroxide (H2O2), superoxide (O2), and hydroxyl radicals (OH-) These molecules cause cellular damage by reacting with lipids, proteins, and DNA 14-19.
The aim of this study was to determine the presence of FOR and antioxidant capacity in the corneal alkali burns and to evaluate the effects of amniotic fluid on healing.