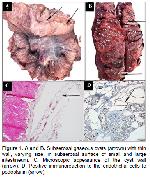
Pneumatosis cystoides intestinalis (PCI), also known as intestinal emphysema, pneumatosis intestinalis, cystic lymphopneumatosis, and intestinal gas cyst, refers to multiple thin-walled endothelial lining pseudocyst formations which are filled with gas sizing from a few millimeters to several centimeters in diameter in the intestinal wall
1,2. It is reportedly a rare incidental lesion in weanling-pig, dog, rabbit, and human beings
1-3. However, clinically these lesions might lead to an incorrect radiological diagnosis of tumor and signs of intestinal obstruction. It might occur in any portion of small intestine, however also involve in the large intestine, mesenterium, and mesenterial lymph nodes
3-5.
The condition in human medicine is associated with a large variety of diseases and clinical conditions in which the loss of intestinal mucosal integrity and/or luminal high pressure usually occur. PCI can be classified in terms of pathogenesis as primary (idiopathic without any obvious cause) or secondary to a wide variety of conditions including; intestinal necrosis, intestinal obstruction, mucosal disruption, increased mucosal permeability, and pulmonary disease 1.
There are mainly 4 sources of gas in the intestinal wall; gas escapes through any disruption of the mucosa, pulmonary gas released from the ruptured alveoli, gas production of some bacteria and excessive fermentation due to maldigestion 6.
PCI is mostly asymptomatic, however, a spectrum of clinical signs including vomiting, abdominal distention, abdominal pain, diarrhea, constipation, and tenesmus was reported in dogs 4,5.
This report presents morphological and immunohistochemical findings of a case of PCI in pig.