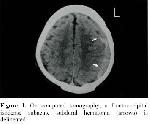
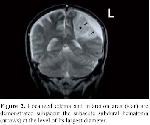
Coexistence of subacute subdural hematomas with TIA is seldom encountered and the real incidence is not known
8. Clinical progression of subacute subdural hematoma with the association of sudden developing transient ischemic neurological symptoms, display a different manifestation as to be a phenomenon. In this phenomenon, the most frequent symptoms are motor aphasia and paresis
4. Likewise, in our case, motor aphasia was associated with right hemiparesis.
The mechanism in the development of TIA in conjunction with chronic subdural hematomas is controversial 8. Welsh EJ reported two cases of chronic subdural hematomas presenting with transient neurological deficits in which cardiac or carotid artery bruits were identified 10. In another case of Kaminski et al, atrial fibrillation was found. Likewise, atrial fibrillation again was found in a similar study of Guptha and Puthrasingham 2. In the etiology of transient ischemic attacks, heart originated emboli are the most frequent etiological factor. Carotid athero-embolus is known as another etiological factor 4,9. Besides, development of chronic subdural hematomas has been reported following anti-aggregation therapy used in order to reduce the incidence of cerebral emboli in atrial fibrillation or carotid atheroma cases 1. Therefore, those transient ischemic attacks reported before are not due to chronic subdural hematomas, but rather due to emboli originating from heart or carotid artery, therefore it is not appropriate to mention under this phenomenon since it leads some pathophysiological controversies. Therefore, it is crucial to make differential diagnosis between these diseases causing transient ischemic attacks.
There are two basic factors in the pathophysiology of this phenomenon 2,6,8,10. 1) Mass effect of the chronic hemorrhage in the subdural space 2) Local cerebral edema caused by hematoma, without necessarily enlargement in the diameter. Furthermore, additionally mechanical stimulation to cortical mantle and even more, the changes in the head position could lead to the development of these symptoms intermittently 6,8. It is obvious that mass effect of the hematoma has a great role in the development of this phenomenon, since recovery in the attacks were achieved after the evacuation of the hematoma 4,7,10. Since no similar phenomenon is observed in most of the chronic subdural hematomas with significant mass effect, anatomical variations in the cerebral vascular structures adjacent to hematoma likely have the main effect in defining the physiopathology.
TIA is a focal neurological deficit lasting 15-20 minutes not extending beyond 24 hours. The neurologic deficit was completely resolved after the first attack in our case. However, discrete from the cases reported before, in our case, hemiparesis was partially permanent despite anti-edema therapy after the second attack. Ischemia progressing to infarction in the region adjacent to hematoma was delineated on 48 hour follow-up MR imaging. Neurological deficits in our cases were transient initially, which became permanent because of the delay in the hematoma evacuation, therefore, we recommend emergent surgical evacuation in these kind of chronic subdural hematomas associated with this phenomenon. The previous cases reported in the literature with a good recovery in TIA after evacuation of coexisting hematoma, all support our hypothesis.